To describe the clinical characteristics and prognosis (hospital mortality at 30 days and 12 months and emergency department readmission at 30 days for acute heart failure) of patients treated in hospital emergency departments for new-onset or de novo acute heart failure (NOAHF) and to compare the patients with those who consult for chronic decompensated heart failure (CDHF).
PatientsNOVICA is a secondary analysis of the Epidemiology of Acute Heart Failure in Emergency Departments registry. We compared demographic variables, baseline characteristics and data from acute episodes and follow-up at 30 days and 12 months of patients with NOAHF and CDHF.
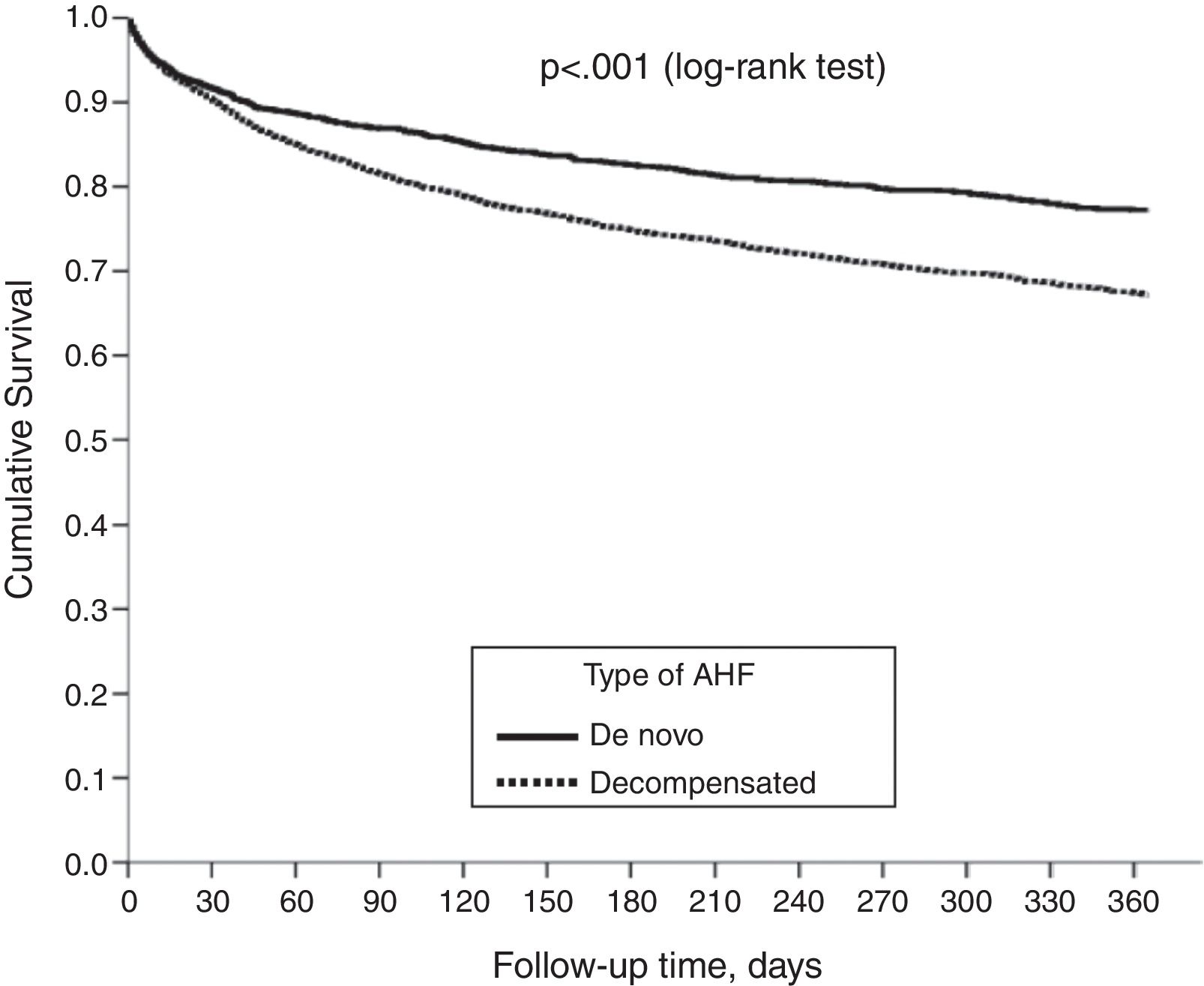
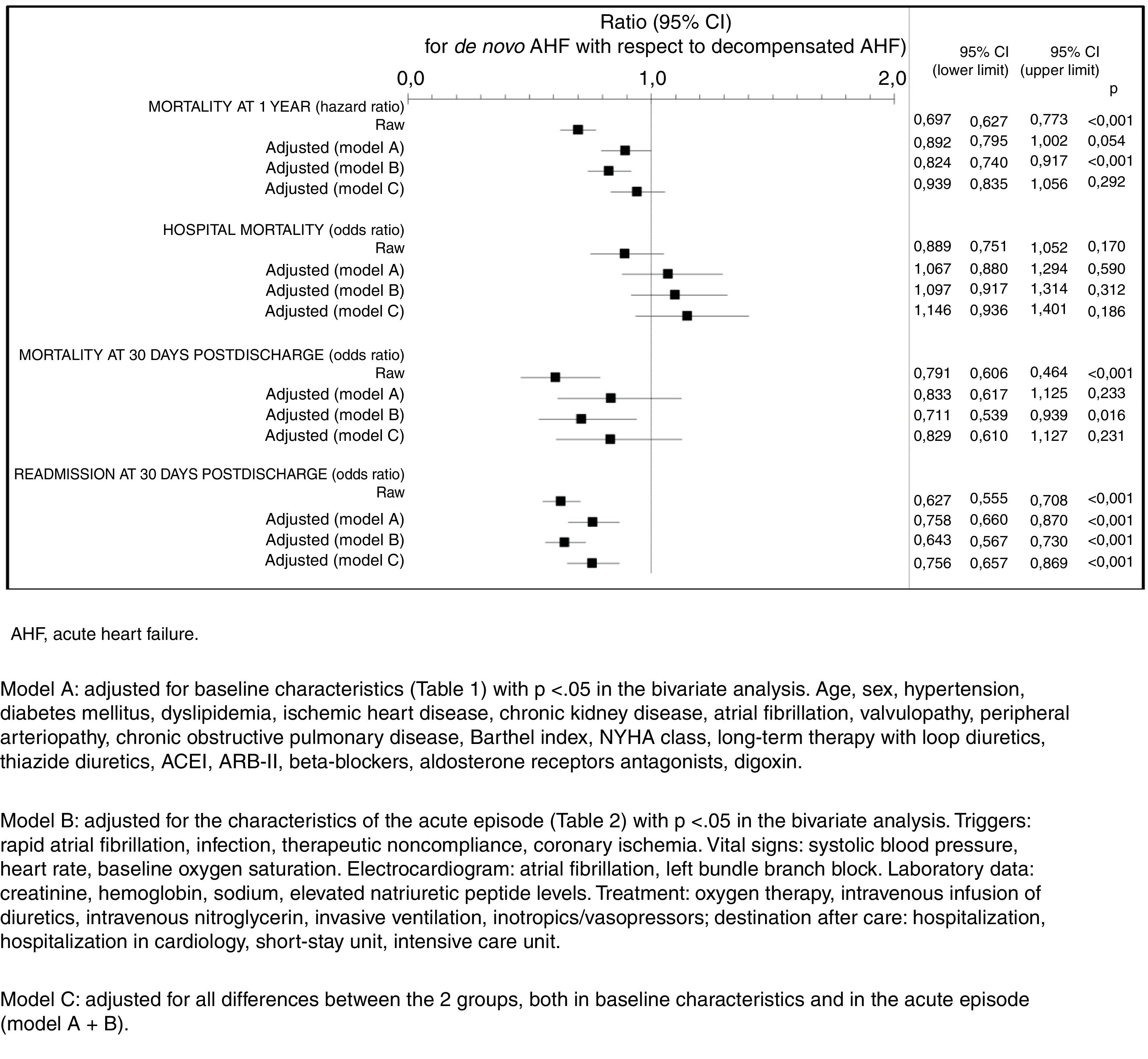
ResultsWe analyzed 8647 patients, with 3288 cases of NOAHF (38%) and 5359 cases of CDHF (62%). NOAHF was associated with lower comorbidity, better baseline state, less severe acute episode data, less use of diuretics in intravenous infusion and oxygen therapy and lower hospitalization rates. The patients with NOAHF were admitted more often to cardiology and intensive care units, and the patients with CDHF were admitted more often to short-stay units. Rates of crude mortality at 30 days and 12 months and readmission at 30 days were higher for the patients with NOAHF. In the adjusted analysis, however, only the rate of readmission at 30 days was lower for NOAHF (p<.001).
ConclusionsPatients admitted to hospital emergency departments for NOAHF show a different clinical profile from patients with CDHF. In the adjusted analysis, there were no differences between the 2 groups regarding hospital mortality, 30-day mortality or 12-month mortality.
Describir las características clínicas y el pronóstico-mortalidad intrahospitalaria, a 30 días y a 12 meses y reconsulta en urgencias a 30 días por insuficiencia cardiaca aguda-de pacientes atendidos en servicios de urgencias hospitalarios por insuficiencia cardiaca aguda de nueva aparición o de novo (ICAN) y compararlas con los que consultan por insuficiencia cardiaca crónica descompensada (ICAD).
PacientesNOVICA es un análisis secundario del registro Epidemiology of Acute Heart Failure in Emergency Departments. Se compararon variables demográficas, características basales, datos del episodio agudo y seguimiento a 30 días y al año de pacientes con ICAN e ICAD.
ResultadosSe analizaron 8647 pacientes, 3288 ICAN (38%) y 5359 ICAD (62%). Las ICAN asociaron menor comorbilidad, mejor estado basal, datos de menor gravedad del episodio agudo: menor uso de diuréticos en perfusión intravenosa y de oxigenoterapia, menor tasa de hospitalización. Las ICAN ingresaron más frecuentemente en cardiología o unidades de cuidados intensivos y las ICAD en unidades de corta estancia. La mortalidad cruda a 30 días y a 12 meses y la reconsulta a 30 días fueron inferiores en pacientes con ICAN. No obstante, en el análisis ajustado solo la reconsulta a 30 días fue inferior en las ICAN (p<0,001).
ConclusionesLos pacientes que consultan en servicios de urgencias hospitalarios por ICAN muestran un perfil clínico diferente a los pacientes con ICAD. En los análisis ajustados, no hay diferencias entre los dos grupos en relación a mortalidad intrahospitalaria, a 30 días ni a 12 meses.
Article
Diríjase desde aquí a la web de la >>>FESEMI<<< e inicie sesión mediante el formulario que se encuentra en la barra superior, pulsando sobre el candado.

Una vez autentificado, en la misma web de FESEMI, en el menú superior, elija la opción deseada.

>>>FESEMI<<<