SARS-CoV-2 fundamentally causes a severe respiratory infection characterised by diffuse interstitial infiltrates. Some cases of myocarditis have been reported as causing arrhythmia, heart failure, cardiogenic shock, and even death in some patients.1,2 The most likely pathophysiological mechanism is multifactorial: from the direct damage of the virus to the cardiomyocytes, the immune response generated by the body against the viral infection, or the hypoxia-induced injury.3
We present the case of a 61-year-old male with a history of obesity who self-referred for symptoms of progressive dyspnoea of five days since onset and was admitted with severe hypoxemic respiratory failure.
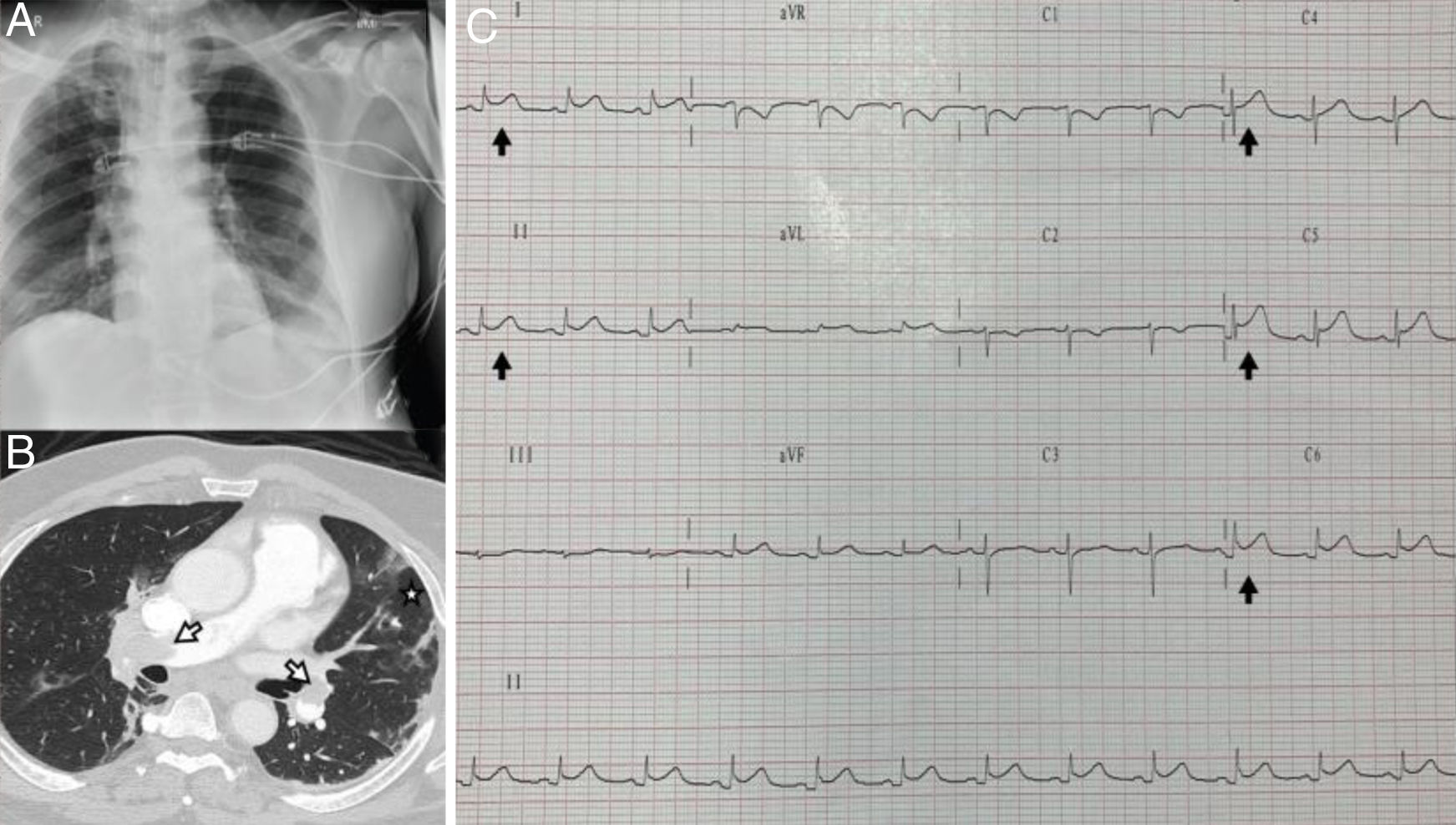
The chest radiography showed bilateral interstitial infiltrate (Fig. 1A). Severe pneumonia due to Covid-19 was suspected and confirmed via PCR. Due to hemodynamic and respiratory instability, orotracheal intubation and mechanical ventilation was required; a transthoracic echocardiogram (TTE) was performed which showed severe dysfunction of the right ventricle with paradoxical septal motion due to overload of the right cavities, in addition to severe tricuspid regurgitation.
With suspected pulmonary thromboembolism, computed tomography angiography (CT angiogram) of the chest was performed, confirming the presence of thrombi in both main pulmonary arteries (Fig. 1B). This clinical situation required high dose catecholamines and elevated oxygen requirements, so systemic fibrinolysis was administered. During admission, a progressive trend towards stabilisation of the clinical picture was observed with improved right ventricular function and normalisation of the cardiac damage markers.
On the seventh day of admission, under sedation and analgesia and connected to invasive mechanical ventilation, the patient presented electrocardiographic changes (ECG) with generalised concave ST elevation (Fig. 1C), confirming elevation of the cardiac damage markers. A new TTE was performed, showing adequate left ventricular ejection fraction (LVEF), with mild to moderate pericardial effusion, suggestive of acute myopericarditis.
The patient showed satisfactory evolution and was moved to the ward 14 days after his initial admission.
In conclusion, SARS-CoV-2 infection can cause systemic involvement beyond respiratory failure, with cardiac complications common during the clinical progress of this disease,4 with elevated morbidity and mortality. Therefore, it is vitally important to be highly aware when preventing and diagnosing these cardiac complications in order to properly manage these types of patients in intensive care units.
Serial ECG analysis, cardiac markers, and echocardiograms are recommended in patients with SARS-CoV-2 infection. Nevertheless, it can be hard to clinically differentiate between cardiac involvement due to sepsis or stress cardiomyopathy or due to a coronary syndrome.5
FundingThis study did not receive any type of funding.
Conflicts of interestThe authors declare that they do not have any conflicts of interest.
Please cite this article as: Pérez-Acosta G, Santana-Cabrera L, Blanco-López J, Martín-González JC. Miopericarditis por COVID-19: A propósito de un caso. Rev Clin Esp. 2021;221:312–313.